Drugs – psychoactive ones, specifically – alter how the central nervous systems of their consumers function. These drugs are illegal or restricted in most countries; but users continue to rise each year globally. Many of them are considered non-therapeutic and widely used for recreational purpose – hence are often abused. Some common psychoactive drugs include cocaine, ephedrine, codeine, cannabis, ecstasy, LSD and so on. Among these, ecstasy – also called MDMA, E, Adam, molly, X, XTC, Mandy and so on, is a widely used party drug and has become increasingly common. It’s not just for partygoers anymore. According to The Global Drug Survey Report 2016, MDMA pills as well as powder are rated as the best drugs based on their value for money.
MDMA of course, is known to cause a feeling of immense euphoria, happiness, and increased sociability – experiences you’re unlikely to have even with considerable solo mental effort. How does the chemical accomplish this? Let’s delve into the effect of ecstasy consumption and the claimed therapeutic potential of the drug.
Related: The Science behind Cocaine
Tracing Ecstasy History
A few decades after its first synthesis by German chemical firm Merck in 1912, merely as an intermediate compound for another production, ecstasy rose to be one of the most popular party drugs in the 1980s. An interesting fact is that before its fame as a party drug, ecstasy was actually tested and even used as a therapeutic drug. The US Army, in 1953, commissioned a study of the behavioral and toxic effect of several chemicals including MDMA.
Alexander Shulgin, also called the Godfather of Ecstasy, was among the first researchers to have studied the psychoactive effects of MDMA in humans. He and his accomplice David E. Nichols published their findings in 1978 and hinted the possible application of MDMA for psychotherapy. MDMA was growing popular among psychotherapists and psychiatrists despite the limited research available on its effect on humans. By early 1980s, MDMA became popular in nightclubs and the recreational market rapidly escalate.
The 1971 UN Convention on Psychotropic substances categorized ecstasy as a Schedule I drug, which poses a serious risk to public health. The criminalization of the drug by several countries like UK and US followed soon after. The ecstasy market suffer enormous decline due to strict laws laid against its use – both recreational and therapeutic. In spite of all these, ecstasy remains one of the most sought after party drug in the twenty first century.
How Ecstasy Gets You High
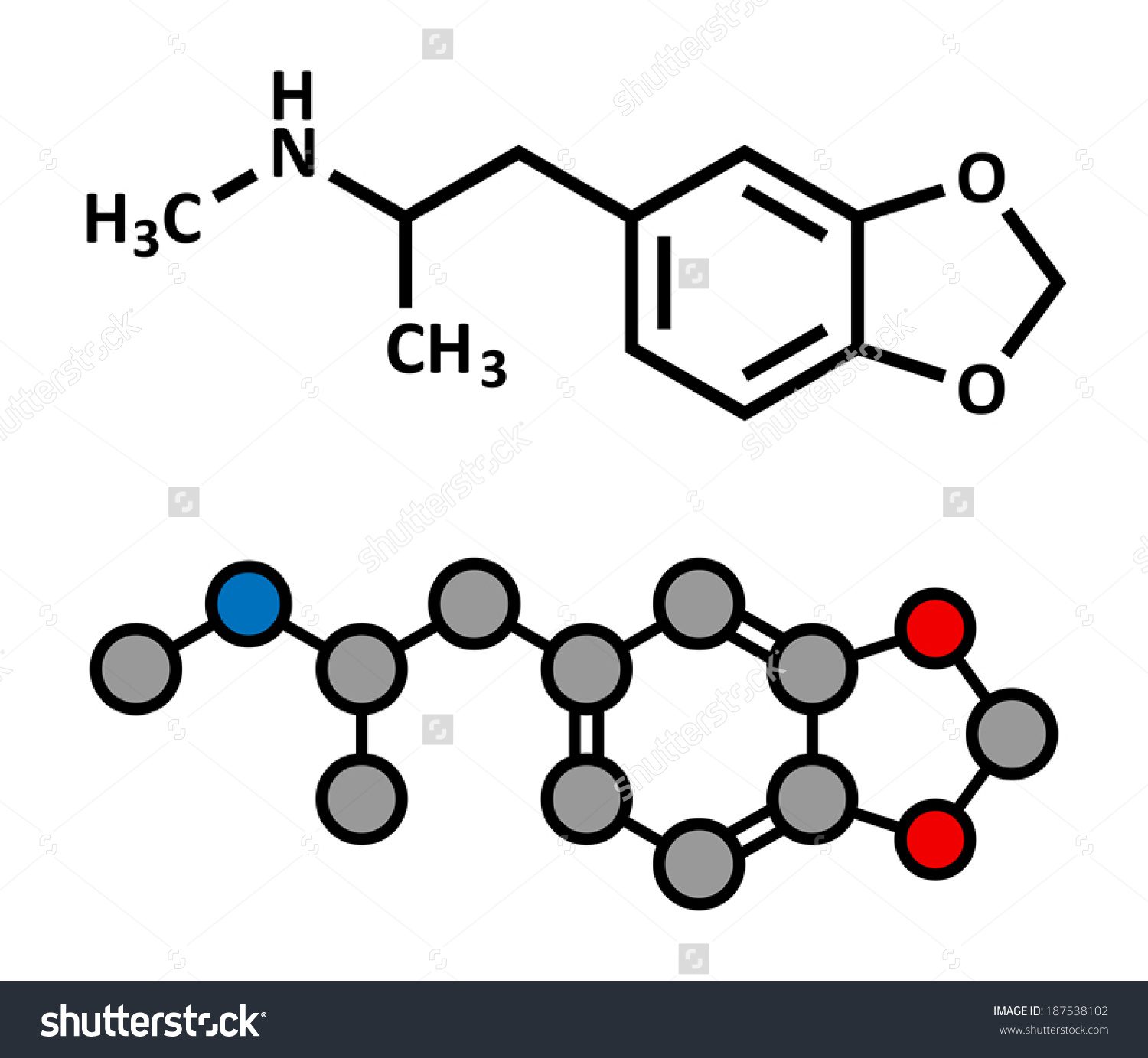
MDMA, or 3, 4-Methylenedioxymethamphetamine, is the major constituent in an ecstasy pill, which may also contain other substances like methylenedioxyethylamphetamine (MDEA), methylenedioxyamphetamine (MDA), or other impurities. When a person consumes ecstasy, MDMA is readily absorbed in the gastrointestinal tract and its effect begins within 30 minutes and peak after one to three hours. MDMA is then partly metabolized in the liver to methyldioxyamphetamine, an active metabolite. It further travels to the heart, which pumps it to the lungs through blood vessels. Then the oxygenated blood further carries ecstasy from the heart to the brain and other organs.
On reaching the central nervous system, the primary action of MDMA is an increase in the release of three important neurotransmitters – serotonin, dopamine and noradrenaline resulting in psychological changes. Dopamine is the brain’s reward chemical – responsible for a sense of satisfaction and happiness. This explains why ecstasy causes a feeling of immense content, increases socialibilty, and uplifts the user’s mood.
Neurotransmitters are chemicals that help in the flow of signals between successive neurons in the nervous system. Most scientific researches on the effect of ecstasy emphasize on the serotonin pathway. We shall try to understand this mechanism.

Serotonin pathways are found at two important areas – in the brain stem and along the spinal cord. As shown in the given diagram, serotonin is present at the nerve terminal of a neuron and is released into the synaptic space by electrical impulses coming from the other end of the nerve. When released into this space, the serotonin binds to the receptor in the next neuron, causing a change in the properties of the receiving neuron – generally decreasing its firing rate. This released serotonin, if not bound to the receptor, is removed from the synaptic space by special proteins called ‘transporters’.
Related: The Science behind Cocaine
MDMA targets and binds to these transporters preventing them from picking up serotonin – causing a surge – a lot of serotonin accumulation in the synaptic space. Hence, more receptors for the serotonin become activated and the brain chemistry is highly altered.
To simplify things – imagine neurotransmitters are responsible for your mood. An excess of neurotransmitters will then cause an extreme version of a corresponding mood. This is what MDMA is accomplishing with serotonin. Somewhat similar effects happen in the case of dopamine and noradrenaline, which are also released in more amounts due to the effect of MDMA.
All these mechanisms results in variety of psychological as well as physiological changes in users. The psychological effects include a reinforced elevated mood, or ‘euphoria’ and a sharpened sensory perception, greater sense of empathy, increase sociability and more. Physiological changes often include dry mouth, stiffness, headache, loss of appetite, insomnia, pupil dilation and others (Cohen, 1995). Eventually after the metabolism rate of MDMA slows down, less serotonin is released which can result in anxiety and depression, and at times, memory loss too.
The Rainbow behind the High
Apart from its use as a recreational drug, ecstasy is known to have therapeutic applications especially in the treatment of post-traumatic stress disorder (PTSD) patients. The past medical use of ecstasy was not well accepted due to the social stigma that ecstasy comes with and the absence of proper scientific researches. MDMA is also known to be less addictive as compared to other psychoactive drugs.

When taken in regulated amount, MDMA reduces fear and increases trust and empathy. This help PTSD patient ermain calm and better engage in psychotherapy. The first completed clinical trial to test the therapeutic applicability of MDMA for PTSD therapy was performed by five American scientists including Michael C Mithoefer, a renowned psychiatrist.
Their report states, “MDMA-assisted psychotherapy can be administered to post-traumatic stress disorder patients without evidence of harm, and it may be useful in patients refractory to other treatments1”. Moreover, the Multidisciplinary Association for Psychedelic Studies has been performing trials for studying effectiveness of ecstasy for PTSD treatment. The earlier trials turn out to be positive and Phase III trial is set to be performed soon. We are waiting for more research to find whether the medical application of MDMA will be safe and reliable in the long run.
We may not be too far from legalization
Many pharmacologists and psychotherapists are optimistic about the legalization of MDA for therapeutic purposes. This will allow the better control of purity and dosage of ecstasy pills. According to the Global Drug Survey 2016, ecstasy quality and purity is on the rise, making it more powerful and more dangerous. Ecstasy pills containing over 250mg of MDMA are now regularly reported – quite unsafe as compared to the 80-100mg pills from in the past decades.
Decriminalization of Ecstasy can lead to better restriction on quality and more accessible treatment for abuse and overdose. Dr. Adam Winstock, founder of GDS, states “Credible conversations that treat people as adults who want to stay happy and healthy and that accept that drugs can enhance a person’s life are needed… Drug laws increases stigma and make it less likely people will seek help and advice.”
As for now, the recreational use and abuse of ecstasy far exceeds the safe therapeutic use. The next time someone mentions about getting high, be sure to think of the chemistry behind it.
Reference: Michael C Mithoefer, Mark T Wagner, Ann T Mithoefer, Lisa Jerome and Rick Doblin (2010) Journal of Psychopharmacology 25: 439–452
